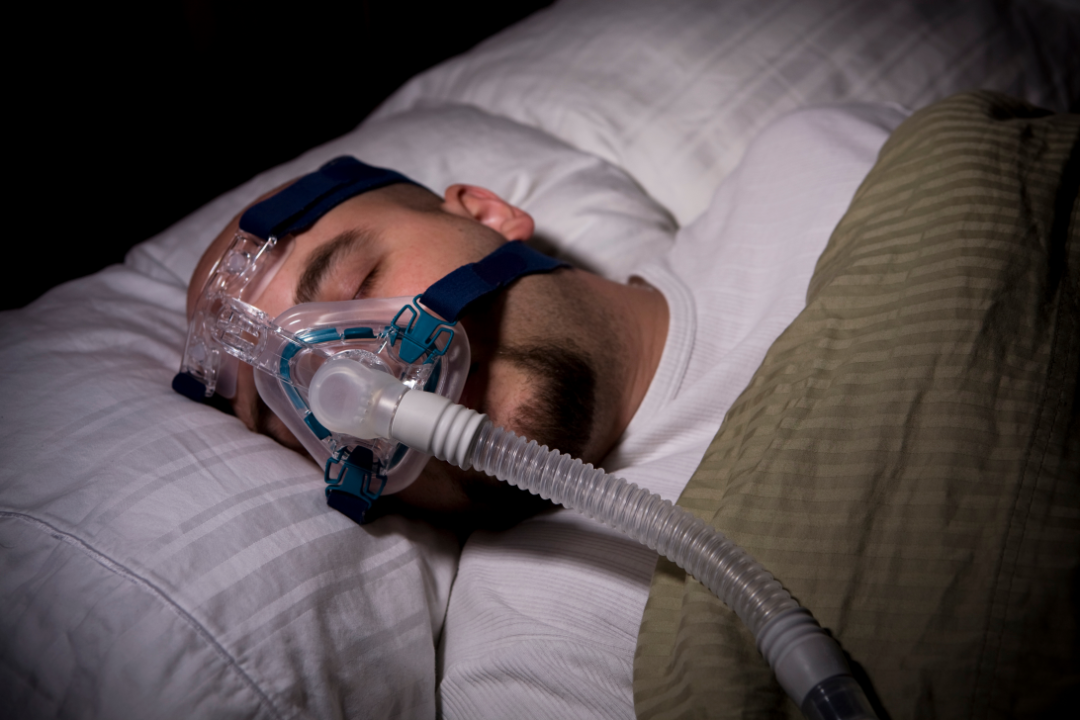
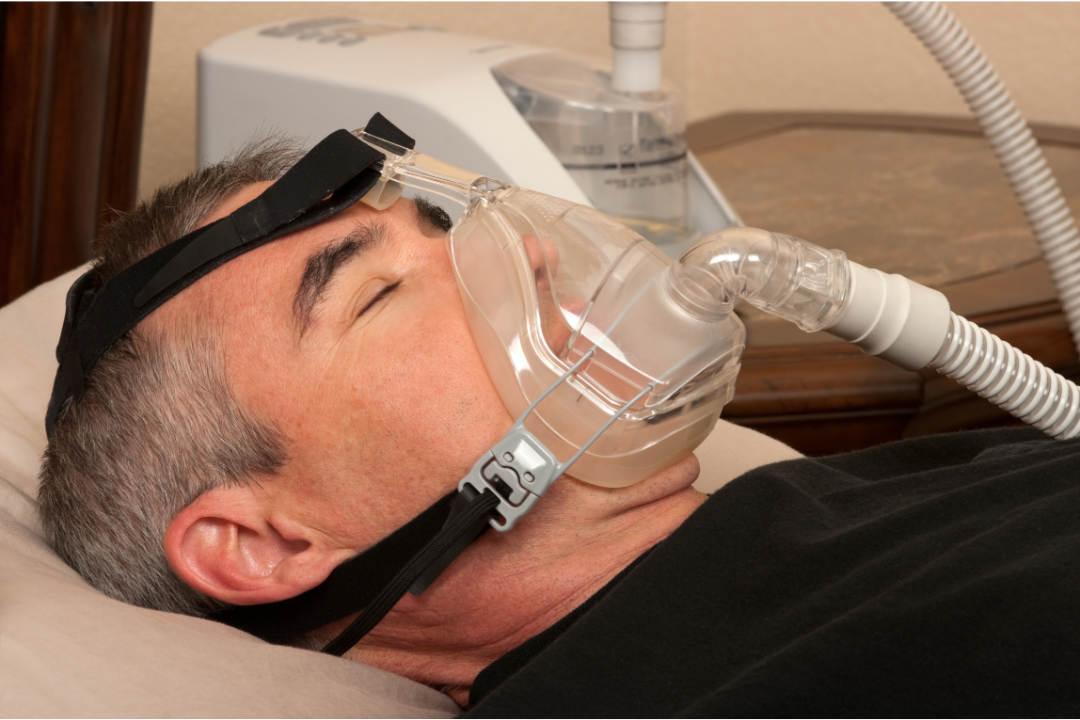
Making your CPAP masks wearing more comfortable
We understand. It might be challenging to use CPAP masks. The mask, the noises, and the air are all foreign to you. Never give up. We’re prepared to assist. Adjust…
How to choose a good sleep position with your CPAP masks
Millions of Australians suffer from sleep apnea, a breathing problem that is often treated with a continuous positive airway pressure (CPAP) machine. CPAP masks come in a variety of styles,…
How CPAP masks work
A CPAP mask is the most often recommended technology for treating sleep apnea problems. Obstructive Sleep Apnea (OSA) is caused by breathing pauses or interruptions, which are usually due to…